A woman suffering from cramps lies in bed holding a hot waterbottle
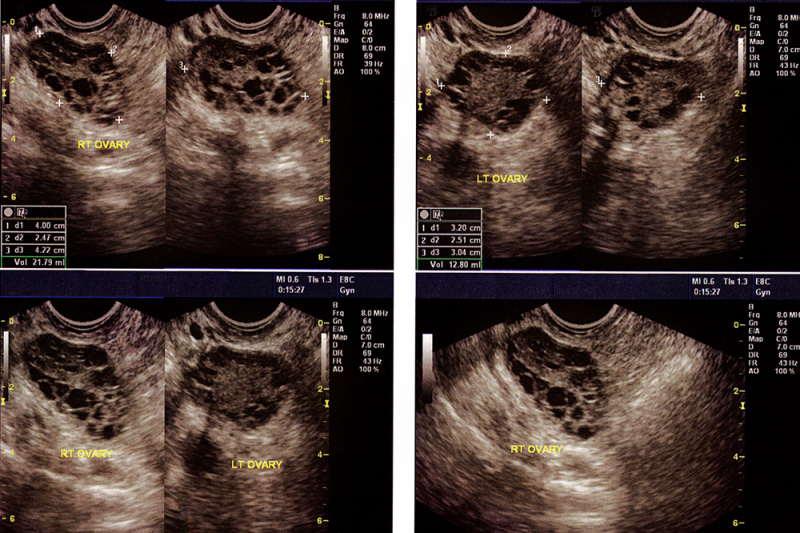
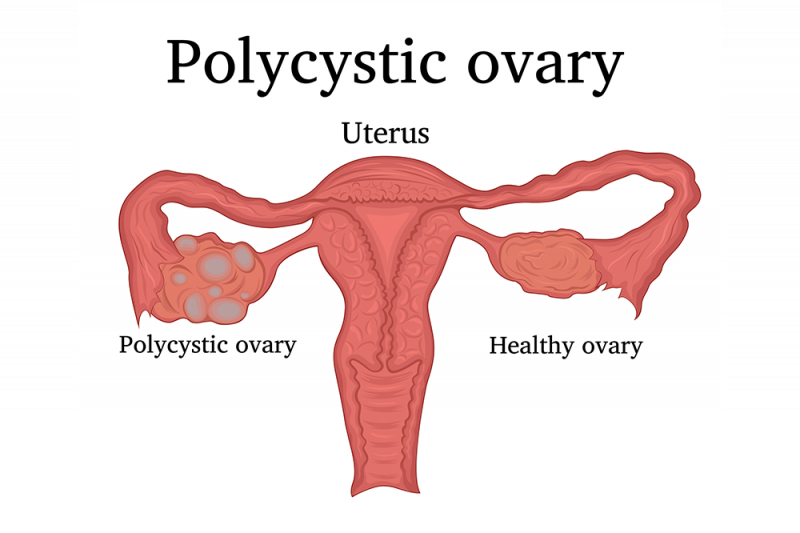
Polycystic ovarian syndrome, commonly known as PCOS, is a complex hormonal disorder that causes cysts on a woman’s ovaries. The cysts are eggs that have failed to properly mature, and on an ultrasound, they look like black dots on the ovaries.
While not often talked about, PCOS is common, affecting 8-13% of women between 15 and 44, with a higher prevalence in women of Asian, African, Aboriginal, and Torres Strait Islander backgrounds.
The exact causes of PCOS are unknown, but it’s thought to arise from an imbalance of reproductive hormones, which can create issues in the ovaries such as eggs not developing correctly, or eggs not being released at all during ovulation.
Early diagnosis and treatment may help reduce the impacts of long-term issues that are commonly associated with PCOS, such as Type 2 Diabetes and high blood pressure.
It’s very common for women to have ovarian cysts – up to a third of all women will have them. So how do you know if you have PCOS?
Signs and symptoms
PCOS symptoms usually present during puberty but they can begin in the early to mid-20s. Some symptoms will last a lifetime, but others will stop at menopause.
There is no simple diagnostic test for PCOS. Women will often have a range of different symptoms, which can include:
- excessive hair on face, chest, stomach or back
- scalp hair loss
- acne
- polycystic ovaries (seen on ultrasound)
- obesity, easy weight gain, or swollen belly
- infertility or reduced fertility
- irregular or absent menstrual periods.
Diagnosis
To be diagnosed with PCOS women generally need to have two out of three of the following:
- Irregular or absent periods
- Acne, excess facial or body hair growth, scalp hair loss, or high levels of testosterone and similar hormones in the blood
- Polycystic (many cysts) visible on an ultrasound.
Women who have immediate family members with PCOS are more likely to also have it, with as much as a 1-in-2 chance of having PCOS.
Diagnosis of PCOS usually involves taking a thorough medical history, conducting an ultrasound of the ovaries and blood tests to determine hormone levels. The type of ultrasound used is a transvaginal ultrasound which involves placing a probe inside the vagina. Transvaginal ultrasounds are used in preference to the usual abdominal ultrasounds as they provide a better-quality image.
Blood tests will indicate if a woman has elevated levels of androgens (male sex hormones) and insulin or any other hormonal imbalances.
Long-term health risks of PCOS
PCOS is associated with the following long-term health risks:
- insulin resistance
- increased risk of the development of diabetes, especially if women are overweight
- cholesterol and blood fat abnormalities
- cardiovascular disease (heart disease, heart attack and stroke)
- endometrial cancer (if there is long-standing thickening of the lining of the womb).
Treatment
If you have symptoms and want more information about how to deal with PCOS, your best course of action is reaching out to your GP and discussing your options.
Treatment for PCOS depends on the symptoms experienced by a woman and whether she is seeking to become pregnant.
For women who are diagnosed with PCOS because of infertility investigations, the immediate treatments focus is on re-establishing regular ovulation to improve the chance of pregnancy.
The aim of treatment for women not wishing to become pregnant soon is to provide relief from the various symptoms.
In the past, treatments for PCOS often only focused on the cosmetic symptoms like acne, excessive hair growth and obesity. However, current treatment for PCOS also seeks to address the long-term health implications such as the increased risk of diabetes and cardiovascular disease.
Living with PCOS
A healthy lifestyle can help you manage PCOS. Eating a healthy diet and exercising regularly can help ease some of the possible physical and mental issues associated with PCOS. Exercising regularly can also reduce your risk of diabetes and improve your chances of getting pregnant.
You can get further help and advice from the following:
- a gynaecologist
- an endocrinologist
- your local women's health clinic
- community health centres
- a dietitian
- an exercise physiologist.
If you are unsure, you can also call 13 HEALTH. You can phone and talk to a registered nurse 24 hours a day, 7 days a week, for the cost of a local call.