
Your bone marrow is constantly working to keep you alive, but do you know what it does?
**A quick warning for anyone with needle phobia – in this episode Dr Fraser details the processes of bone marrow harvesting, which involves needles. If you’re squeamish with needles, you might want to skip from 19:00 to 24:55.**
My Amazing Body is a podcast where we explore interesting, unknown and misunderstood parts of your body with help from medical experts and stories from real Queenslanders.
This episode is all about the bone marrow. Dr Chris Fraser, Paediatric Oncologist and Director of the Bone Marrow Transplant Program at Queensland Children’s Hospital, explains what bone marrow is, what it does and why it's so important to your health. He talks us through conditions that can affect the bone marrow, and how bone marrow transplants work. We also hear from Vince, a Queensland man who donated his bone marrow to a child he didn't even know, in an attempt to help save their life.
Meet our guests

Dr Chris Fraser is a Paediatric Oncologist and Director of the Bone Marrow Transplant Program at Queensland Children’s Hospital. Dr Fraser spoke with us about what bone marrow is, how it impacts your health and what happens when it’s impacted by disease.

In 2015, Vince donated his bone marrow to try to help save the life of a sick child. He explains how the procedure happened and why he decided to undergo the operation.
Episode materials
Audio is great, but some things are best seen as well as heard. These materials provide more information about topics we touch on in the show.
The pelvis
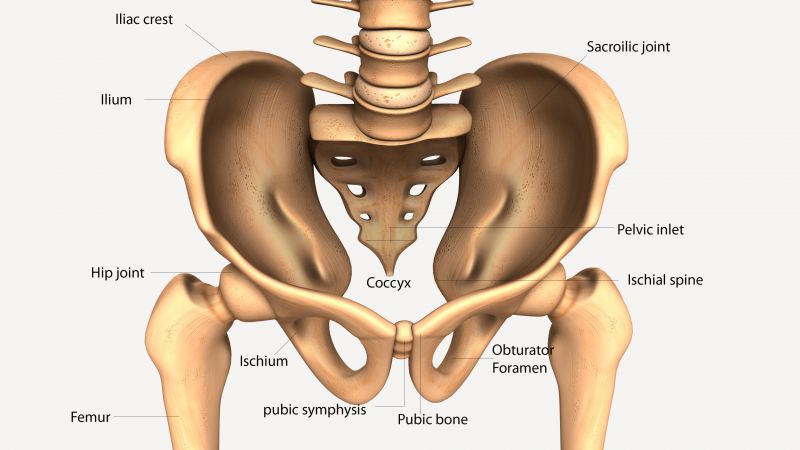
The bones of the pelvis hold the red blood marrow used for bone marrow donations. At 20:26, Vince talks about how his bone marrow was harvested from his pelvis, near the iliac crest. You can see this area in the diagram above.
Bone marrow failure syndromes
While leukaemia might be a more well-known cause of people needing bone marrow transplants, as Dr Fraser explains, bone marrow failure syndromes or BMFS are serious illnesses that might be treated with a bone marrow transplant. More information about BMFS, including conditions like aplastic anaemia, can be found through the Leukaemia Foundation and Maddie Riewoldt’s Vision.
Becoming a bone marrow donor
Inspired by Vince’s story? You can find more information about donating bone marrow from Australian Red Cross Blood Service and the Australian Bone Marrow Donor Registry.
Transcript
Host: What are you willing to do to help others? Would you stop a stranger in the street to let them know they dropped something? Would you help someone you saw struggling with their shopping bags? Would you go under a general anaesthetic and let doctors suck out some of your bone marrow, to give a stranger a second chance at life?
Hi, I'm Elise. Welcome to the latest episode of My Amazing Body, where we explore interesting, unknown and misunderstood parts of your body. Today we're learning all about your bone marrow. We'll find out what it does, how it works and what happens to your body it's not working properly. We'll also find out what it takes to be a bone marrow donor, from a Queenslander who donated his bone marrow to a stranger, and how you can sign up to be a potential donor, too.
Dr Fraser: I'm Dr Chris Fraser, I'm a Paediatric Oncologist, or a children's cancer specialist and the Director of the Bone Marrow Transplant Program here at the Children's Hospital in Brisbane.
Host: Dr Fraser works at Queensland Children's Hospital, working to save the lives of children with serious diseases like leukaemia. He gave us the low down on what bone marrow is and why it's so vital for your body.
Dr Fraser: I usually explain that, you know, bone marrow is essentially a factory that makes your blood cells. There's three main types of blood cells; there's red blood cells that have haemoglobin in them that carry oxygen around your body. And there are white blood cells and they're important for fighting off infection; they make up the immune system. And there's little cells called platelets which are important for stopping bruising and bleeding. They're the three main types of blood cells that the bone marrow produces and that's really its main function – to make those blood cells.
Host: As the name suggests, your bone marrow lives inside your bones. Red bone marrow, which is the type that produces blood cells, is located mainly in the central bones of your skeleton, like your pelvis, sternum, cranium, ribs, spinal vertebrae and scapula, which you might know as your shoulder blades.
Every second of every day, this bone marrow is hard at work making new blood cells. There are billions of blood cells in your body, and as they reach the end of their lifespan, your bone marrow has to replace them with fresh cells.
Dr Fraser: Why does it make so many blood cells? The body is constantly regenerating those blood cells. Each different type of blood cell has a different life span; the red blood cells on average live for about three months but some of the white blood cells and platelets actually only live for three or four days and so the bone marrow has got to generate a whole new supply of those cells every three or four days. And if you look at the number of those cells in your body it's, you know, it's enormous. I think if we look at white blood cells there's about 2 billion white blood cells per litre. And the bone marrow has to make a new supply of them every three or four days. So, the bone marrow is a pretty efficient factory; it has to make a lot of cells.
Host: If you've ever done a shift at a restaurant kitchen or on a factory line, you'll know what it feels like to be constantly churning out products all day. But for your bone marrow, the work shift never ends. It’s a 24-hour production line, and it operates every day for your whole life.
Diseases and conditions that affect bone marrow are relatively rare, but when they strike, they can be very serious, because bone marrow plays such an important role in your body. Dr Fraser talked us through some of the conditions that can affect bone marrow in children and adults.
Dr Fraser: You know there's a lot of diseases that can affect the bone marrow. In paediatrics, the most common thing that we would see is actually leukaemia. You know leukaemia is a type of cancer of one of the immature forms of white blood cells that live in the bone marrow. And when you develop a cancer or a tumour, those cells just divide out of control and they fill up the bone marrow space so that the normal bone marrow can't work. And that's essentially what happens with leukaemia.
Host: Every year in Australia, leukaemia affects 21 out of every 100,000 children aged 0 to 4, 10 per 100,000 aged 5 to 9 and 12 per 100,000 aged 10 to 14. While leukaemia patients make up only a small proportion of the children at Queensland Children's Hospital, they are among the sickest, and often have to stay in hospital for treatment for a long time.
Dr Fraser: There are lots of different types of leukaemia, and you know broadly speaking you can divide them into acute leukaemias and chronic leukaemias, and the two main groups of acute leukaemia are acute lymphoblastic leukaemia or acute myeloid leukaemia.
Host: When diseases like leukaemia is called acute, it means that is appears suddenly and grows quickly. Chronic disease appears more slowly and gradually develops over time. Dr Fraser says children are more likely to develop acute forms of leukaemia, while chronic leukaemia is more common in adults.
Dr Fraser: So, in acute lymphoblastic leukaemia the cancer cell is a type of cell called a lymphoblast which is one of the immature forms of white blood cells. And so, acute lymphoblastic leukaemia is the most common type of childhood cancer. There are peaks in incidence in different age groups and there's a peak in the 2 to 4-year-old age group, so it is more common in that age group. Acute myeloid leukaemia on the other hand the incidence increases throughout life, essentially, in a fairly linear fashion, so that's a type of leukaemia that becomes more common as you get older.
The chronic leukaemias – chronic lymphocytic leukaemia or chronic myeloid leukaemia – are much more common in adults and very rarely seen in children.
Host: While leukaemia is the most well-known, there are other diseases and conditions that can affect the bone marrow. At Queensland Children's Hospital, Dr Fraser also treats children with other diseases affecting their bone marrow and other parts of their body.
Dr Fraser: There are certainly other diseases. There's a group of diseases that we term bone marrow failure syndromes, and they can be divided up into conditions that are acquired or conditions that you're born with that are inherited. The most common form of acquired bone marrow failure would be something that we call severe aplastic anaemia.
And then there's the inherited bone marrow failure syndromes are things that we primarily see in children, although there are some patients who won't be diagnosed until adulthood. And there's a whole range of those conditions that essentially are inherited, usually in what we call an autosomal recessive fashion, so a mum and a dad might be carriers of a particular mutation in a particular gene – they're not affected in any way but if their children inherit the copy of the gene from each parent that's got the mutation, which has a one in four chance of that occurring, then they can be affected with a range of very severe bone marrow failure syndromes.
Those syndromes often come along with other manifestations, so there might be abnormalities in certain bones or particular facial appearances or things like that. So, there's a group of those conditions that as I said are rare, but you know important causes of bone marrow failure in children.
And those conditions also, apart from presenting the problems of not making enough blood cells, because that bone marrow is under stress, it makes them more prone to develop leukaemia. And so those children have a much higher risk of developing leukaemia as well.
Host: Are you ready for this episode's mystery body part? See if you can guess what the body part is from the clues given. We'll reveal the answer at the end of the episode.
What am I? I'm padded with fatty tissue to act as a shock absorber for your body. Over time, my skin might dry out and crack if you don't look after me. If you have podophobia, you might be scared to see me! The bone I cover is called the calcaneus, and it's the largest bone in your foot. Do you know what I am?
Host: For patients with diseases like leukaemia or bone marrow failure syndromes, a bone marrow transplant might be their best hope for a cure. During a bone marrow transplant, bone marrow is taken from the body of a healthy donor and transplanted into the patient.
Dr Fraser: So, a bone marrow transplant, which is essentially replacing your diseased bone marrow with a healthy donor's bone marrow, certainly is an option for many of the bone marrow diseases that we've talked about. Bone marrow transplants can be done for leukaemia and that probably does remain our most common indication to do a bone marrow transplant. However, there's an increasing proportion of patients who have what I would term non-malignant, or non-cancerous conditions who also have life threatening diseases that affect their bone marrow, who also bone marrow transplant is often the only curative therapy for those conditions.
Host: Having a bone marrow transplant comes with significant risks for the recipient, something that Dr Fraser and his colleagues have to consider when offering the treatment to patients and their families.
Dr Fraser: It comes along with a whole bunch of you know risks and there's a real risk of dying from the complications of a bone marrow transplant. So, we reserve bone marrow transplants for those children where we have identified that our chances of curing the leukaemia with chemotherapy alone are not as good as we would like them to be. And you know, probably once you start getting below maybe a 60% chance of curing the cancer with chemotherapy alone that's when we'd start saying, well, it's worth accepting those risks of a bone marrow transplant and going ahead with a bone marrow transplant assuming you can find an appropriate donor.
Host: If you need a transplant, you can't take bone marrow from just anyone. You need to receive bone marrow from someone whose marrow matches yours, and it turns out finding a match can be pretty complicated.
Dr Fraser: So, to find a donor, looking for a donor you're really looking, we do something called HLA typing. HLA stands for human leukocyte antigens. Leukocyte just means white blood cells and antigens means proteins that are expressed on the surface of the cells. And these HLA, or human leukocyte antigens, we can test and define the antigen or the protein type at 10 different spots or what we call loci. And you inherit five of those from your mother and five from your father. That's called, the ones we measure are called HLA A, B, C, DR and DQ. And at each of those proteins there are hundreds of variations that can occur, and you can imagine that if you've got 10 proteins each of which could be several hundreds of variations, that the possible combinations are almost infinite really, there's just innumerable combinations.
And that's by design, you know, evolution has done that and made each of our bodies unique. The principal of that HLA system is that your own immune system should recognise that unique signature on your cell and say, 'yep that cell's meant to be here, I don't need to get rid of it'. In just the same way that the immune system can get rid of cancer cells, those cancer cells shouldn't have that unique signature on them so the immune system should be trying to get rid of those cells.
Host: Finding a good match increases the chances that the bone marrow transplant will work and reduces the chance of life-threatening complications for the recipient.
Dr Fraser: Because the chances of the bone marrow transplant being successful are directly proportional to how well matched the donor is, because the complications, the main complications of a bone marrow transplant either rejecting the cells or the new immune system attacking your body causing something called graft verse host disease, are dependent upon how well matched the donor is.
Host: When it comes to finding a donor, a patient's siblings are Dr Fraser's first port of call, with a one-in-four chance that full siblings will be a match.
Dr Fraser: So, you can imagine that there are millions and millions of combinations of this HLA signature and there are HLA antigens, what we call minor histocompatibility antigens, which we don't even measure for the purposes of finding a donor.
So, it's a very complex, incredibly complex system. So, the first place that we look is within the family. A full sibling will have a one-in-four chance of being matched to a child or an adult who needs a bone marrow transplant. And that's because its simple probability: you inherit 50% from your mother and 50% from your father, to get the same 50% is a one-in-four chance for each child.
Host: Some patients don't have siblings or have siblings who aren't suitable donors. In this case, the worldwide search for a matching donor begins.
Dr Fraser: So, if you don't have a matched sibling donor, then the next step is really to look at the unrelated bone marrow donor registries around the world and we have a bone marrow donor registry in Australia and there are many others around the world. I think we're up to 16, 17, maybe 18 million people who are on those registries, and there is a database and you can search and you can see whether you can find a match.
Your chances of finding a match in that registry depends upon your ethnicity because your HLA type runs with your ethnicity. So the Caucasian population have certain HLA types and equally Asian populations or African, Indigenous Australians they all have unique HLA types, and there are certain ethnicities that are not well represented on the unrelated bone marrow registries in Australia, the Indigenous population are not well represented, and if we don't find a family match it's very challenging to find a donor on the unrelated registries.
Host: In Australia, the Australian Red Cross Blood Service operate the Australian Bone Marrow Donor Registry. When a person signs up to donate blood, they're also asked if they would like to register as a potential bone marrow donor. If they do, their tissue type and details will be saved on the database, which can be accessed by registry services worldwide when a patient is in need of a matching donor.
We spoke to Queensland man Vince, who, after years of being a registered bone marrow donor, got the call to say he was a potential match for patient in need of a transplant.
Vince: Many years ago, and I'm talking about probably at this stage 1993. So, we're looking 26 years ago now. My now wife and I were walking past police headquarters here in Brisbane City, and we decided we should to the right thing as the community spirited people that we are and donate blood.
Off the back of that one donation, in 2015 I was contacted by the Australian bone marrow donation registry to tell me that I was a match for a sick child in relation to a bone marrow.
Host: It had been a long time since Vince had signed up as a potential bone marrow donor, but he didn't think twice when it came to agreeing to donate his bone marrow.
Vince: I can remember that day very well. It was probably one of those days that you never think is going to happen or is never going to come. But I had a great feeling of elation that something I had done so many years ago, that I was able to be in a position to help somebody.
Host: The chances of a registered donor getting the call to donate are quite slim. Every year, only 1 in 1,500 potential donors will get the call that they might be a match.
Vince: I was aware that there was a greater likelihood that I wouldn't be selected than I would be selected. But I think that from my point of view, and certainly from my wife's point of view, if you had an opportunity to help somebody or be in a position to help somebody, we certainly want to engage with that and become registered as donors.
Host: After a potential bone marrow donor is found through the registry, they undergo a series of tests to make sure they're the best donor possible for the recipient, that they're healthy and ready to make the donation.
Vince: Initially there was blood tests that I had to undertake, which I did that day actually at the Red Cross.
Based on those blood tests and the great contact with the Australian Bone Marrow Donor Registry, through the Red Cross, they were able to get back to me fairly soon. I remember giving a number of vials of blood at a later time after participating in doing a chest x-ray and a few other investigative techniques that were managed by the department of oncology at the Royal Brisbane Hospital for the purpose of ensuring that I was the best match in the circumstances for the recipient.
Host: Once a donor has been found and screened, there are actually two ways they can donate their bone marrow. The first procedure is the one most people are aware of through TV and movies, where doctors use a needle to suck bone marrow out of the donor's pelvis bone while they're unconscious. This is the procedure Vince underwent. Dr Fraser explains how it all works.
Dr Fraser: As a sibling or a parent or an unrelated donor who is going to donate bone marrow for a bone marrow transplant there are two options of the ways that it can be donated. One is we can collect bone marrow itself, so that's something we call a bone marrow harvest, and to have a bone marrow harvest you need have a general anaesthetic, and need to make sure your fit and healthy enough to do that.
And while you're asleep two doctors usually will be on either side of you, you'll be placed on your stomach and then your pelvis bone – you can sort of feel, at the back there the pelvis has two big wings so if you picture the skeleton at the pelvis there's these two big wings – and we can feel the back of those wings pretty easily through your skin. And we just put a pretty big needle through the skin into the bone and screw that through the outer surface of the bone and then put a syringe on the end of the needle and you can suck out bone marrow.
Host: That all might sound pretty intense, but surprisingly Vince says he felt pretty good after his donation.
Vince: My procedure involved extracting bone marrow from the iliac crest, which is in the lower part of your back. There has to be a general anaesthetic for that. So, you're prepped as an inpatient, but for a day surgery. As I said, painless, very simple procedure. Only takes a number of minutes to affect the actual outcome and the extraction of the bone marrow. I can remember eating quite a bit of food in the day surgery unit afterwards, which was, yeah, couldn't ask for better care from the hospital staff and the Red Cross.
There was a slight ache in my lower back. Maybe that was age or maybe that was just from the procedure itself. But I was up and about doing normal things within a day.
Host: The amount of marrow needed for the transplant depends on the age and size of the patient receiving it. In Vince's case, his recipient was a child, so a smaller amount of marrow was taken compared to an adult recipient, which may have helped him make a swift recovery.
Dr Fraser: We generally only you know take a few millilitres with each puncture of the needle. To do a bone marrow transplant you need ideally about 15mls per kilo of the patient's weight. So, you know, if that's a 20-kilo child you only need 300mls of bone marrow, that's pretty achievable. If it's a 80 kilo adult you know you're talking about 1 and a half litres plus of bone marrow. And you know, that's a tougher ask for someone to donate that much bone marrow so.
Host: Dr Fraser says that while some donors might feel a bit sore after their donation, the whole procedure is very safe and shouldn't cause any lasting discomfort for the donor.
Dr Fraser: It's a very safe procedure; we obviously couldn't do it on healthy donors be they related or unrelated if it wasn't very safe. And when we do these bone marrow harvests on siblings of children, toddlers even or 5, 6, 7, 8-year-olds they don't, it's a day case, they come into hospital for the day they don't get admitted over night, they don't require a blood transfusion afterwards and most of them are really running around that afternoon. Doesn't really knock them around too much.
In adult donors for whatever reason, maybe they've got tougher bones, but the pain and discomfort afterwards is more significant and can last for a week or more, being quite uncomfortable having had this big needle put in your pelvis bone that many times.
Host: For Vince, after a day or two off work, he was back to normal, only now he lived with the knowledge that he might have helped save the life of a sick child.
Vince: I think I took the day of the procedure off work and one other day. And apart from there, there's no ill effects. I haven't had any physical complications or anything that you may associate with having a procedure. It's a very simple, painless, and really effortless procedure on the behalf of the donor.
It's a painless, effortless procedure on behalf of the donor – I can't emphasize this enough. That was my experience. And certainly, I've donated blood, I've donated plasma, I've donated platelets. And I'd have to say one of the easiest donations of all of that would be bone marrow.
Host: Dr Fraser says that the second way bone marrow can be donated is through a process similar to donating blood, where bone marrow stem cells are collected through an IV.
Dr Fraser: So, you want these bone marrow stem cells, and the other way you can get them in by something we call an apheresis procedure. This involves giving the donor an injection of a medicine called GCSF – it's a growth factor – and that pushes the bone marrow stem cells out of the bone marrow into the circulation. And you have that and on the fifth day you can have two large IV canula put in each arm and your blood comes out of one arm, goes through a machine called apheresis machine and those bone marrow stem cells can be filtered off and the rest of your blood gets put back into you through the other arm.
And that doesn't involve needles in your back, it doesn't involve a general anaesthetic, but it does involve having this growth factor injection for five days beforehand that does have some rare incidences of some complications.
Host: When it comes time for the patient to receive their bone marrow donation, Dr Fraser said the transplant doesn't happen in an operating theatre, like some people might expect.
Dr Fraser: From the patient's perspective many people think, ‘Oh, a bone marrow transplant means that you have to inject the bone marrow directly into the patient's bones or something and it's an operation’. In fact, a bone marrow transplants not really an operation at all. The patient comes in and is admitted to hospital and is placed in a special isolation room to try and minimise the risk of infections.
They will all have had what’s called a central line placed, so they've got a line in a big vein in their neck that can be used for giving drugs and taking blood tests and giving blood transfusions, that sort of thing. But it's also used to give the bone marrow, so the bone marrow is just run in like a blood transfusion. The patient will come in, be admitted and have what we call their conditioning which is either just chemotherapy or a combination of chemotherapy and radiation. That usually runs over on average probably about a week, probably a bit shorter sometimes a little bit longer. That's designed to wipe out their own bone marrow, kill some leukaemia cells ideally, if it's being done for leukaemia, supress their immune system so they don't reject the new cells. They're the main jobs of the conditioning regimen.
Then the cells are just run in as I said just like a blood transfusion through the central line and those cells make their way to the bone marrow spaces, they set up camp there and the factory hopefully starts working again.
And it takes anywhere between two to four weeks before you start seeing those first blood cells being produced. So, we'll be doing a daily blood count during this time and the white blood cells are the ones we see being produced first. And you know it will go from zero to 0.1, 0.2 and at that point in time you know that the cells are being grafted and they haven't been rejected and you have to wait until they get up to being closer to normal levels. And in the meantime, you have to monitor your patient for all the complications that can occur, complications related to the high doses of chemo and it's affect upon various organs, infections which are a really big risk. Once the cells are in graft that risk goes down a bit but it doesn't actually go away for quite some time; that new immune system takes at least six months or so to learn all the things it needs to learn to give you decent protection against infection.
Host: For unrelated donors like Vince who have been found through the registry, laws that protect both their privacy and the privacy of the recipient and their family mean that donors don’t often know the outcome of their donation.
Vince: They've been as fulsome as they can be in relation to how the patient's going. Because that's a big thing for a donor to know that once you've made the donation, you still have that connection I suppose in a way with the recipient. And you'd really like to know what's going on. They're bound by privacy, and I could not fault them in relation to their ability to maintain my privacy and the recipient’s.
Well, I certainly asked. And to the extent that they could, the Red Cross were able to tell me that the recipient was doing well, which was very uplifting for me. I suppose for the donor the act of giving is the important thing. But it's certainly nice to know that that act has had a positive outcome.
Host: Vince encourages all eligible Queenslanders to sign up to the registry and potentially save a life.
Vince: I'd certainly make them aware of the Red Cross and the Australian Bone Marrow Donor registry, they have fantastic information.
I certainly promote not only at my workplace, but in my personal life to others and friends that I know, because it is such a great experience. And the opportunity to help somebody, that lies within us. So, the way we're made up physically and biologically, you have the opportunity to help somebody. I took that opportunity. And I think it's one of the best days and opportunities in my life to have that experience.
Host: If you're interested in registering to become a bone marrow donor, you can visit the Australian Red Cross Blood Service website at donateblood.com.au for more information. We've included the link in the shownotes for this episode.
For Dr Fraser, bone marrow is a big part of his daily job. It can be tough, but rewarding, work.
Dr Fraser: So, in terms of how many bone marrow transplants we would do, on average, in a hospital our size it would be 25 to 30 a year. And roughly half of them are for kids with leukaemia and half for kids with non-malignant or non-cancerous conditions. So yeah, I guess it depends how you look at it whether that's a big number or not. It’s a very intensive procedure for each of those 30 kids who have that transplant a year.
It's a challenging job, because it probably is about the most intensive type of treatment that you can go through in terms of the potential risks and complications and the complexities of those complications. And the duration of time that you're in hospital, even when things go completely smoothly, when things don't go smoothly and complications occur, then your hospital stay can be extremely prolonged at times.
But obviously you know when it all works out well, which it does the majority of the time, it is very rewarding to see these kids when they come back. I see them very frequently; in the initial period after transplant they have to come to clinic twice a week, and then once a week and then once every fortnight. But when you get to the stage where you're only having to see these kids every six months or twelve months or so and they're doing very well and their disease is cured it's extremely rewarding.
Host: Thanks for joining us for another episode of My Amazing Body. Before we wrap up, did you guess our mystery body part for this episode? The fleshy covering for your calcaneus bone is your heel! Congratulations if you figured it out.
My Amazing Body is bought to you by Queensland Health. With special thanks to our expert guest Dr Chris Fraser, bone marrow donor Vince, and my podcast colleagues – Lauren our researcher, writer and producer, Carol our audio technician, Helen on sound effects and Dan our music guru. Special thanks to the media team at Children's Health Queensland and the Queensland donor coordination team at The Australian Bone Marrow Donor Registry