
How well do you look after the trillions of bugs that live on your skin?
My Amazing Body is a podcast where we explore interesting, unknown and misunderstood parts of your body with help from medical experts and stories from real Queenslanders.
This episode is all about your skin microbiome – the collection of bugs that live in your skin. With dermatologist Dr Tania Zappala, we talk everything from creating a healthy environment for your skin microbiome, to why the bugs are there in the first place and how they work to help keep your skin healthy. She also describes how dominant microbes can cause skin conditions like eczema and acne. Psychologist Emma Kefer talks about the mental health impacts of skin conditions, and Queenslanders Tracey and Alana tell their tales of out-of-balance skin microbiomes.
Meet our guests

Tracey speaks about her son’s eczema, which first started showing when he was a baby.

Alana details the physical and mental effects of having severe childhood eczema.
Episode materials
Audio is great, but some things are best seen as well as heard. These materials provide more information about topics we touch on in the show.
Eczema
Throughout the podcast, Dr Zappala talks about eczema one of the most common skin conditions effecting Australians. You can find out more information about eczema at Health Direct. If you think you or your child have eczema, it’s important to see your GP or a dermatologist for appropriate treatment.

At 6:42, Dr Zappala talks about a ‘filaggrin defect’, that can cause eczema. You can read more about this here, and see how it works in the diagram below.
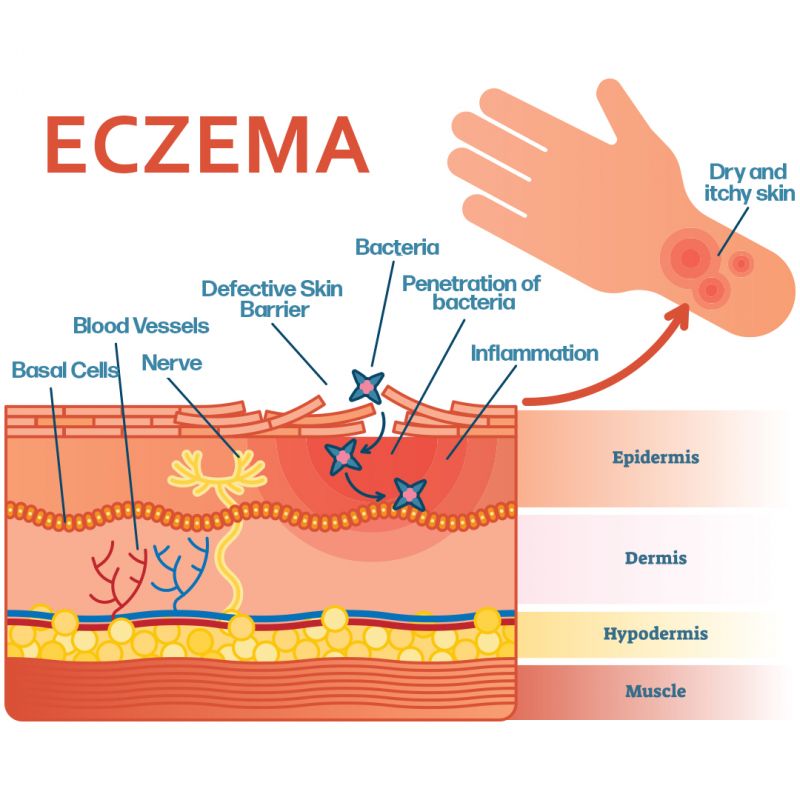
For more information about how the skin microbiome can effect conditions like eczema, and how changing the microbiome might be a useful treatment method, read The Conversation’s Applying live bacteria to skin improves eczema.
You can find more information about eczema at the links below:
Australasian society of clinical immunology and allergy: Eczema
Pregnancy, Birth & Baby: Eczema in children
Acne
At 20:00, psychologist Emma Kefer talks about the effects conditions like acne can have on people’s mental wellbeing. You can find more information about the study Emma references, from the British Journal of Dermatology, here. For more information about acne, visit Health Direct, All About Acne or see your GP or dermatologist.
Episode transcript
Host: I want you to picture a pond. On the top of the pond you can see ducks paddling around, a frog fly fishing on a rock and dragonflies landing on the colourful flowers of a Lilly pad. Underneath the surface, fish swim through the shallows, reeds float in the currents and worms wriggle in the silt. If you had a microscope, you could see teeny tiny creatures munching on the moss.
When everything is in balance, all the living things in the pond thrive. But if there is imbalance, like too much algae on the pond's surface blocking the sunlight, or not enough ducks to eat snails and worms, then the pond's ecosystem, and all its life forms, suffer.
Hi, I'm Elise. Welcome to the latest episode of My Amazing Body, where we explore interesting, unknown and misunderstood parts of your body. Today, we're learning about your skin microbiome.
You might not know it, but your skin works in a similar way to the pond you were just imagining. All over your skin are heaps of different types of living microorganisms and when they're in balance, so is your skin. This is called your skin microbiome, and to make it easier to picture, in this episode we're going to call the microorganisms that live there 'bugs'.
Dr Zappala: There are at least trillions of bugs, which is a hard concept to get around. Other people have sort of postulated that there are at least 10 times more bugs on our skin than human cells making up our body, which is quite amazing to consider in that we may be more bug than human.
Host: That's Dr Tania Zappala, a dermatologist who works at Queensland Children's Hospital. Dr Zappala spends every day working with Queenslanders and their families to help balance and look after their skin microbiomes.
Dr Zappala: Do you know that most people who I launch into a discussion about bugs on our skin, I think within their gut, have worked it out themselves. It just sort of all clicks into place when you say, 'So we're covered in bugs right, and we need to balance them back out'. And everyone sort of sees how the point in which they've to seeing me goes, 'that makes sense'.
Host: Before she treats a patient's skin condition, Dr Zappala says it's important to remember that most of the bugs on our skin are helping us to stay healthy, and we really want them to be there.
Dr Zappala: There are two main things that the bugs on our skin do for us and one is to interact with our immune system and either keep it in check or help it along, and the other thing really is to keep the bad bugs out. And those are very simple concepts, but it makes sense; when we've got healthy skin, what we know the key is that there is a diverse population of many, many, many different bugs, including bacteria, viruses, fungi, mites.
Host: The bugs on our skin aren't just freeloaders coming along for the ride. Some of them are preventing infections and others can even stop cancers from growing.
Dr Zappala: The way that the organisms keep things in check is really fantastic. They can interact directly with our immune system. They can talk to our cells directly and make antibiotics from our body naturally. They can even survey our cells for broken bits of DNA and stop cancers before they happen. So, these bugs have really got our back and in a sense the question that I think it would we be able to function without them?
Host: Because some of the bugs in our skin microbiome are so useful, Dr Zappala doesn't ever want to wipe a patient's microbiome clean. Instead, like Goldilocks, she's trying to get the balance of different bugs on the skin just right.
Dr Zappala: It's quite incredible; a healthy skin biome is very, very diverse. When we get into trouble, we’re into an area where we've got a dominant organism that's taking over. And what usually we want is to bring back to a diverse group or community of organisms and we've still got the dominant bacteria, for example the Staph aureus in eczema in play, but they're just kept in place by everybody else.
Host: Dr Zappala says one of the tricky things about working with the skin microbiome is that everyone's group of bugs is different.
Dr Zapalla: The key message is that everybody's microbiome is different and reacts differently and although something might work for someone else, it's not going to work in all situations.
Something that was unique, that came out of all the research that's happened over the last ten years, is that people can have really, really healthy microbiomes and they can be completely different to the person sitting next to them with a really, really healthy microbiome. And that creates challenges in itself.
Host: All sorts of things can have an impact on the balance of your skin microbiome, from dry weather, to the medications you take or the kind of moisturiser you use. Just like in the pond you imagined, if conditions favour one type of organism in your skin microbiome more than the others, it can start to take over. If you've ever had a skin condition like eczema, acne or dandruff, that was a sign that your skin microbiome was unbalanced. And once the balance in your microbiome has shifted, it can be easy for a skin condition to snowball.
Dr Zappala: When the bad bugs get out of control we call that dominance, and they tend to have tricks up their sleeve to keep them in power. For example, Staph aureus in eczema, once it takes control, it can then create environments that replicate the original starting out of eczema.
Our skin barrier is like a brick wall and there's a defect in eczema called a filaggrin defect and that is as thought the mortar in the brick wall is not there. So, the skin still looks like a brick wall, but given any little change in the balance the immune system underneath the brick wall can see through the gaps and can see what's happening on top and gets upset. Then staph aureus starts taking advantage of that, then it starts to create a toxin which actually causes more defect in that wall and causes more holes and starts creating more of the innate eczema. So, then we compound the problem and get worse eczema and things start to get out of control very quickly.
Host: Chronic skin conditions caused by an out-of-balance skin microbiome, like eczema, can be debilitating. Dr Zappala says that while we might think about skin health as a “surface level” problem, balancing skin conditions can have a huge impact on her patients.
Dr Zappala: I'd really like people to know that your skin is important. Many people suffer because they think that it’s not affecting them, and you know what? Your overall health has to be in balance and you might find that actually your skin is affecting you more than you know and your quality of life would improve if we could get this right for you.
Host: In particular, Dr Zappala says she sees a lot of patients and their families who are exhausted by the condition they're dealing with.
Dr Zappala: People often ask me why I wanted to paediatric dermatology and really it comes back to the family unit and just seeing a family come in in distress and hopefully a few weeks later be able to be happy, healthy and go off into the world. Being able to give back what they deserve to be able to be giving to the world. These are mums and dads and brothers and sisters and then the child who's itching all night; no-one here's getting any sleep. And if we can get everything back in balance, then there's five people who can have good relationships and happy times and this really gives a lot of value to getting your skin condition treated correctly.
Host: We spoke with Queensland mum, Tracey, who, like many of the patients Dr Zappala works with, has been battling to control the eczema on her young son's skin. Tracey told us about the toll eczema has taken on her son, and also herself.
Tracey: My son is five. He showed his first signs of eczema when he was about 3 months old, and it really flared up a lot once we introduced solid food.
Host: As a baby, Tracey's son had eczema on his cheeks. Now he's five, the eczema mainly occurs on the insides of his knees and elbows.
Tracey: He definitely knows that it's there, and there will be times particularly around the changes of seasons that he'll have really obvious huge, red patches around the inside of his elbows and the backs of his knees, and he'll just be itchy and it's hard for him to sit still in class and deal with that when he's just, I can't imagine being itchy like that all the time. It would be really frustrating.
Host: Tracey says that while well-meaning people would used to ask her questions about his eczema what she found most difficult was the worry about just how much eczema was affecting her son's overall health.
Tracey: Yeah, lots of people would sort of ask what was going on with his face when he was little, because it was quite a prominent thing, being on his face not just on his you know, trunk and his arms and legs. It wasn't something I could cover. And so people would mention it a lot and ask questions about what was going on.
What did bother me was that it looked uncomfortable at times. There would be periods where it was flaring up a lot and I was more personally worried. Not worried about what people think, but more worried about he might be in pain, and there's not much I can do about it. And he's always been a rotten sleeper, and even now he's, you know, still at 5 wakes me up for a good hour every night. So, it's a lot to do with that itchiness and the sensations on his skin. It just kind of disrupts him. Because he's just not able to get enough restful sleep at night. We do everything in terms of the good routine and he's in bed early, but yeah, he wakes during the night or he wakes up really early in the morning and yeah, it has a big impact on his own resilience and ability to cope with things.
Host: For Dr Zappala, satisfaction comes from not just treating her patient's skin microbiome and skin condition, but all the flow-on affects this can have for their overall wellbeing.
Dr Zappala: Having a baby come into clinic with eczema is often a potentially hugely rewarding situation for me. Because I feel with a few facts and points of education the whole family can really benefit.
Host: Tracey encourages other parents to seek medical help if their child has a skin condition like eczema.
Dr Zappala: I would say, listen to your doctor. Don't bog yourself down in weird internet research and try to find alternative cures. Honestly, the stuff that's been proved by science is going to help you. And seek specialist care if your GP doesn't know enough about it.
Host: Are you ready for this episode's mystery body part? See if you can guess what the body part is from the clues given. We'll reveal the answer at the end of the episode. What am I? You’ve got two of me, though on some people the two might reach together to make the appearance of one. If you remove me completely, other people might find it hard to recognise you. Bits of me fall out all the time, with each individual part lasting about four months. I help to keep the sweat out of your eyes. Do you know what I am?
Emma Kefer is a psychologist who works at Queensland Children's Hospital in the Child and Youth Mental Health Service Consultation Liaison.
Emma: So, we can think of our team as looking at the mind-body relationship, how our physical health impacts on our mental wellbeing and also then how we are feeling emotionally effects our physical health. We look at the interplay of those things.
Host: The tiny bugs on our skin affect us on a microscopic level, but can also have big impacts on our overall health. We spoke to Emma about how she sees skin conditions affect the mental health of her patients.
Emma: So if someone is negatively impacted by problem with their skin, you might see changes such as low mood, feeling depressed, social withdrawal, or avoidance from social activities. So, if there was a person who liked to go out with their friends on the weekends, go to the movies, was engaged in a lot of online chatting and then they didn't want their face to be seen, they didn't want to leave the house, that would be a sign that something has changed. And it could be a range of issues and it's really important to make contact with that person and try and understand what's going on for them. They might experience increased anxiety and fear of negative reactions from others and that might be shown in terms of comments about 'oh but what will other people think', and attempts to actively cover up the skin condition.
Host: She says that treating skin conditions as though they are really only "skin deep" can overlook the broader impacts they might have on a patient’s health.
Emma: It's important to know that our skin is our biggest organ and the bond between our skin and mind has very early beginnings, tracing right back to when we were all infants and we had the close skin-to-skin relationship between a new born baby and mother. And so, it's an essential part of life and the skin plays a very important role in our development and in protecting us.
So, for young people, we work with young people up to the age of 18. And there's no time like adolescence – it’s is the most important time for us in terms of worrying about acceptance from peers, belonging, negative evaluation from others, fitting in and the influence of peers is incredibly strong, probably stronger than any other time in life. So, when we meet people not only are they dealing with very challenging medical conditions and the consequences of those but also trying to navigate their social environment and school and relationships as well.
So, the kinds of problems that people will present are ranging from adjustment, stress anxiety, depression. For parents, they might see social withdrawal, a lack of interest in things that their child was previously interested in and a preoccupation with how they look and needing to cover up whatever the problems are that they're having.
Host: Alana, a young Queensland woman with a history of severe childhood eczema, says that as a kid, her condition affected her confidence and ability to make friends.
Alana: When I was growing up, I had super severe eczema. I've pretty much had it my entire life. I don't remember at what age it started, it was just kind of always there.
I loved school and I always really enjoyed being there, but it definitely affected my lunch breaks and playing with other kids, running around. Especially like, on hot summer days and getting the confidence to go up and play with other kids, knowing that they might think that I'm contagious.
Host: She says that her eczema changed the way her peers looked at her, but it also affected the way she saw herself.
Alana: I have memories of just being in so much pain, trying to not scratch. But the need to scratch was overwhelming. So much so that, you'd try so, so hard not to scratch. And when you did, it would give you a tiny bit of relief, but after it would just be so incredibly painful. And I would scratch so much so until it bled, so the backs of my legs and my arms were just like red raw.
So, I think while it was super uncomfortable, there's also an aspect of vanity to it, that, I didn't want to look different to other people, and I didn't want other people to look at me differently. So, it was a real challenge both psychologically and physically.
Host: Even though it might be a bit tricky or awkward, Emma recommends people caring for someone with a skin condition – whether they're a parent, a sibling or a friend – talk to them if they think it's affecting their mental wellbeing.
Emma: The thing we would always recommend is to have an open channel of communication. One of the common problems people say is 'I just don't where to start, what to say, I don't want to make it worse by commenting, do you think I should just say nothing? And we would always recommend that even if it feels hard, it's really important to learn how to communicate with your family member or your friend, and that can be as simple as saying something like, ‘I know you're going through a tough time, I'm here to help, what might be something that we could do together?'
Host: Alana agrees.
Alana: For parents who have kids with eczema…if you haven't ever had eczema yourself, just taking the time to listen to them and to understand how they're feeling about it. And also start conversations. And make them actively involved in their treatment and their treatment options. And keep in mind how it might be affecting them emotionally, not just physically.
Host: Have you ever noticed that you get sweaty when you're nervous? Well, that extra moisture is going to have an effect of the bugs that live in your skin microbiome. Emma Kefer says that the connection between our skin health and our mental health can be complicated, because our mental health can affect how well our skin is, and vice versa. Some common skin conditions can be made worse if a person is experiencing emotional turmoil.
Emma: So, these will be things like acne, hair loss, eczema and dermatitis, excessive sweating, allergies and itching, psoriasis and rosacea. So, we know that those problems have a physical cause and then what's happening for a person emotionally impacts on how that symptom is expressed so it might get better, it might get worse depending on what's going on in their emotional world.
Host: This can become a vicious cycle, because studies have proven that skin conditions can then have a negative effect on people's mental health.
Emma: The second category would be where the skin conditions contributes to the development of a mental health problem, so for example severe acne, which can cause low self-esteem, may cause depression and anxiety and there was a recent study quoted, I think it appeared in one of the local papers about an overseas study looking at adults with acne, where it was found that people have a significantly increased risk of depression in the first five years after diagnosis with particular risk in the first year. And that was when the risk for diagnosis of depression was at its highest I think it was 63% higher risk compared with people without acne.
Host: The study Emma is talking about was published in the British Journal of Dermatology in 2018. Over 100,000 people with acne were studied and it showed that they were at significantly higher risk of developing a major depressive disorder after being diagnosed with acne. The problem was so bad, researchers recommended that any physicians diagnosing a patient with acne, should be on the lookout for signs of mental illness as well. And it make sense, doesn't it? When we don't feel like we look our best, and when the problem seems out of control, it can make us feel really bad about ourselves.
It's clear that the little bugs on your skin can make a big difference to your health, so what can you do to look after them and give them the best environment to thrive in? We asked Dr Zappala to give us the low-down on keeping your skin microbiome in balance, starting with how to avoid an out-of-balance microbiome.
Dr Zappala: Some of the triggers that make a microbiome lose its diversity and have a dominant organism go rogue are natural things that happen over life. The microbiome changes significantly from when you're born through childhood, and the most amount of change happens when you get extra oils and sebum production in teenage years and early twenties. And then it starts to stabilise. So, these natural changes can throw things in and out of balance. We then can layer upon that natural irritants which are in the environment, sweat, urine, faeces for babies and nappy rash.
There's also issues with simply occluding your skin with too much heavy product, for example thicker make-up versus breathable make-ups. We also have things that directly interact with our immune system and cause allergies and these are problematic for our skin.
Host: For people experiencing conditions like acne, it can be tempting to scrub the skin to remove the offending bacteria. But Dr Zappala says this isn't the answer and can cause a lot more harm than good.
Dr Zappala: Scrubbing your face with a face washer and soap actually completely obliterates your microbiome and you’re left with a dry empty space in which things can get out of balance very quickly.
Host: If you're keen to look after your skin microbiome, it helps to start by looking at the bigger picture. Have you been eating well, drinking plenty of water and getting enough sleep? If not, your skin microbiome might be paying for it.
Dr Zappala: So, if people really wanted to take of their microbiome, they would be looking at all avenues of their life and keeping everything, really, as simple as possible and in balance as possible. Sleep deprivation is an epidemic in society at the moment, and that leads to poor diet, smoking, alcohol issues and these sorts of things just throw our microbiome right out.
Host: Dr Zapalla says that when it comes to skincare and what we put on our skin, keeping it simple is key for promoting a health microbiome.
Dr Zappala: I don't want this to sound too overly simple, but, really, the number one and number two things is to keep your skin moisturised and to keep it protected from the sun. Whenever I get asked this by my patients, I really don't want them to feel like I'm selling them a cliche, but all of the science on the microbiome and the preceding science before that comes back to, 'and then if we hydrate our skin appropriately, everything comes back into balance'.
Host: As well as thinking about hydration, Dr Zappala urges Queenslanders to think about what they're using to clean their skin. If a soap is advertised as killing 99.9% of germs, what effect will that have on the skin microbiome?
Dr Zappala: The general principle is that we need to cleanse our skin of irritants and allergens, but we don't want to overdo it. The idea of killing 99% of germs on your skin is maybe not the right concept to follow.
The number one problem in dermatology at the moment is in the increasing amount of people that are suffering from dry skin or irritated skin conditions like eczema. And the absolute number one thing that we get them to do when they walk in the door is to stop all harsh soaps, to stop all antibacterial, antifungal soaps and go with something very, very simple that is essentially a soap-free wash.
Host: And if you do have a skin condition that's causing you grief, or you're caring for someone who does, it's important to follow your doctor's directions about medication use.
Dr Zappala: A myth that I'd really like to bust is that steroid creams harm your skin. It's a really important one because like everything there's two sides to the story, and certainly there is a steroid cream can harm your skin side. The steroid preparations that we have on the market in Australia, and the way we use them, we have fewer problems than we used to 50 years ago. In this way, there's really good evidence that anti-inflammatory creams bring our microbiome back into balance in the very challenging situation of eczema. And it’s a very important tool that we have for eczema, and we need to use it.
Host: Remember Tracey, our mum from earlier? She said learned this lesson the hard way, and now urges parents not to follow in her footsteps.
Tracey: So, there was a long time where I was really anxious about using steroid creams on this tiny, little baby's face, and then we just kind of went through this intensive period and because I'd been so hesitant in the past, it prolonged the treatment time. Whereas if we'd just gone in hard at the start it might have just cleared it up earlier and had less steroid exposure over the long run.
So, we do still use the steroid cream from time to time. But I'm not as hesitant in using it, and I know that if we just, you know, get in there and give it a good week of treatment, rather than prolonging for ages.
Host: Research about the skin microbiome, how it affects our health and how we can affect it, is still ongoing. There's a lot yet to learn, which is something Dr Zappala finds exciting.
Dr Zappala: Something that's important about the microbiome that we're just starting to understand is that we have trillions of bugs that have our back, and they're on our back, and they're on our front and they're everywhere. They are really looking out for us and we do need to learn how to respect them. And, that's going to be the trick, over the next little while, while we work out what all this means...
Host: Did you guess our mystery body part for this episode? The two sweat-catching parts of your body are your eyebrows! Congratulations if you figured it out.
Thanks for joining us for another episode of My Amazing Body. My Amazing Body is bought to you by Queensland Health. With special thanks to our expert guests: Dr Tania Zappala and Emma Kefer, Queenslanders Tracey and Alana for sharing their stories, and my podcast colleagues - Lauren our researcher, writer and producer, Carol our audio technician, Dan our Music Guru and the media team at Children's Health Queensland.

