Protocol for timely transfer of care in emergency departments
Protocol number: QH-HSDPTL-025-1:2021
Effective date: 01 October 2021
Review date: 01 October 2024
Supersedes: Nil - version 1.0
On this page:
- Purpose
- Scope
- Transfer of patients between QAS and emergency department
- Supporting and related documents
- Definitions of terms
- Approval and implementation
- Version control
1. Purpose
This Protocol outlines the mandatory processes for ensuring timely access for patients, who present via Queensland Ambulance Service to a Hospital and Health Service (HHS) hospital for emergency assessment and care.
2. Scope
This Protocol applies to all Department of Health and other employees working in or for HHSs. This Protocol also applies to all organisations and individuals acting as an agent for HHSs (including Visiting Medical Officers and other partners, contractors, consultants, and volunteers).
3. Transfer of patients between QAS and emergency department
The timely transfer of patients off stretcher into the Emergency Department is essential to enable Queensland Ambulance Service (QAS) to respond to the needs of people in the community. The time between presentation of a patient by QAS to an Emergency Department triage point and the transfer of the patient to an Emergency Department bed is described as ‘patient off stretcher time’ (POST).
The key performance indicator pertaining to the transfer of patients is POST of less than 30 minutes.
3.1 HHS requirements
HHSs will ensure:
- Patients are triaged on arrival at the Emergency Department.
- Hospitals assume overall responsibility for patient care from the time of triage.
- The Emergency Department (ED) will aim that patients arriving at an HHS Emergency Department (ED) by ambulance will be received by HHS staff into the appropriate ED treatment area with completion of clinical handover within 30 minutes.
- A suitable area within the Emergency Department is provided for QAS staff to support patients who are awaiting transfer off stretcher.
- Patients who arrive via QAS and:
- remain on stretcher for 30 minutes require a review each 30 minutes to formulate and revise a plan for handover. This is to be communicated to the clinically relevant Emergency Department and QAS staff members. At this point, escalation processes in response to demand within the HHS will be triggered as outlined in the “Protocol for Managing Capacity of Queensland Public Hospitals”.
- have been waiting for transfer off stretcher for at least one hour, may be offloaded to enable QAS officers to respond to Triple Zero calls from the community as clinically assessed by the ambulance control centre. This is to be undertaken at the direction of an on-site senior medical officer, in consultation with the senior nurse, taking into account:
- individual patient acuity and risk
- consideration of all waiting patients within the Emergency Department
- Emergency Department resources
- individuals waiting for an ambulance in the community.
- Appropriate ambulance patients are transferred to the waiting room or alternative area under the care of the HHS.
- Clinical handover occurs immediately upon the patient being transferred off stretcher.
- Patient handover procedures are adhered to, including recording of the time the patient is transferred off the ambulance stretcher onto the hospital bed, in the clinical record by HHS nursing/medical staff within the Emergency Department.
- Processes are in place to ensure the availability of emergency department treatment spaces, e.g. cleaning and restocking.
- HHS staff will work collaboratively with QAS to assist in times of surge.
- A graduated escalation procedure to more senior staff supports 24 hours/day management of access issues.
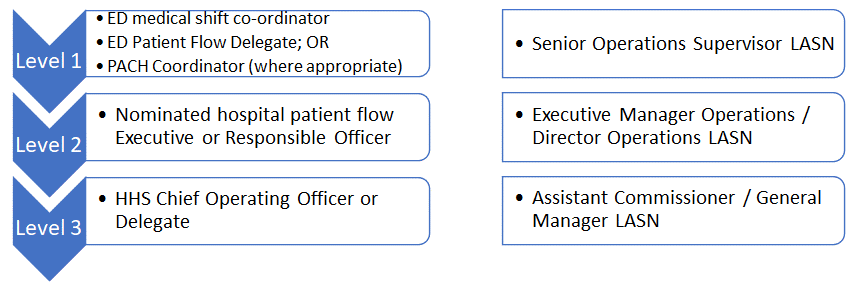
- Suitable escalation processes are in place to identify hospital bed capacity when required to respond to Emergency Department activity, as outlined in Diagram 1.
Diagram 1: QAS escalation levels
3.2 Communication with Queensland Ambulance Service
- The HHS will establish and maintain a HHS-QAS liaison group consisting of relevant HHS Executives, other HHS staff and the QAS LASN. Roles of this group shall include (but not be exclusive to): identifying data trends, trend analysis, case review, and solution design. In some larger HHSs, it may be appropriate to also have a facility-based group reporting to the HHS-QAS liaison group. The HHS-QAS liaison group will report to the Patient Access Advisory Committee established by the Director-General.
- Communication and collaboration will occur between the HHS and QAS during times of surge to manage demand and capacity.
- During these periods of surge demand, the HHS may escalate a Request for Assistance to the QAS when access block is evident.
- Key communication points include:
- QAS escalation Level 1,2 and 3 as per Diagram 1;
- Patient on stretcher > 1 hour is reported to the on-call officer for the HHS.
4. Supporting and related documents
- Hospitals and Health Boards Act 2011
- Relevant local policies or procedures related to demand management and escalation.
- National Safety and Quality Health Service Standards September 2012
- Australasian Triage Scale Policy, Australasian College for Emergency Medicine
Authorising Health Service Directive
Patient Access to Care Health Service Directive
Procedures, guidelines, protocols
5. Definitions of terms
| Term | Definition / explanation / details | Source |
|---|---|---|
| Triage | A triage system is the basic structure in which all incoming patients are categorised into groups using a standard urgency rating scale or structure. | Emergency Triage Education Kit, Australian Government, Department of Health and Ageing. |
Acronym table
| Acronyms | Full title |
|---|---|
| HHS | Hospital and Health Service |
| LASN | Local Ambulance Service Networks |
6. Approval and implementation
Protocol Custodian: Healthcare Improvement Unit, Clinical Excellence Queensland
Approving Officer: Deputy Director-General, Clinical Excellence Queensland
Approval date: 23 September 2021
Effective from: 01 October 2021
7. Version control
| Version | Date | Prepared by | Comments |
|---|---|---|---|
| 1.0 | 23/09/2021 | Healthcare Improvement Unit | Protocol for Timely Transfer of Care in Emergency Departments developed in consultation with key stakeholders. |