
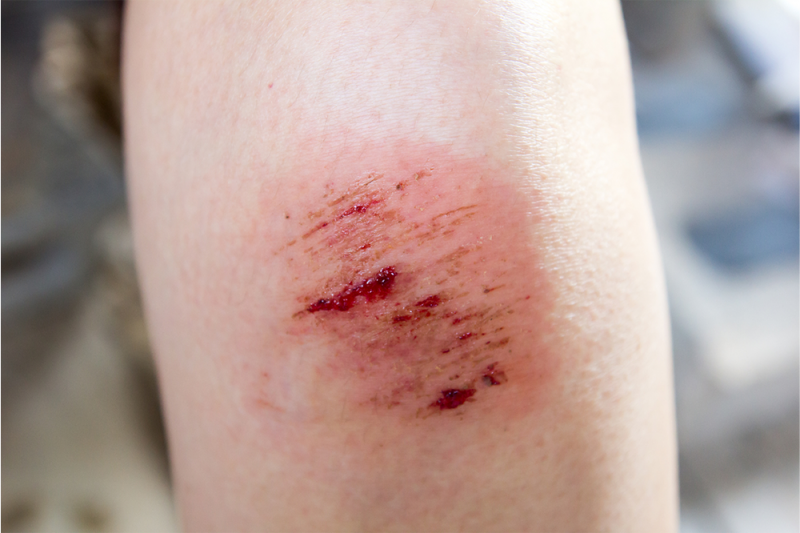
A woman in a red t-shirt puts a dressing on a minor wound on her leg
You may have heard of it by the scary tabloid name.
Necrotising fasciitis is a rare and very serious infection. It can spread rapidly in the body and lead to sepsis, shock, organ failure and death.
Necrotising means causing the death of tissues. Fasciitis is inflammation of the fascia, collagen-based soft tissues that surrounds muscles, nerves, fat and blood vessels.
It happens when bacteria invade the soft tissue and fascia. They multiply quickly, releasing toxins and enzymes that cause blood clots in the blood vessels. This leads to the death of the tissues in your skin and muscles and the tissues under your skin.
Quick and accurate diagnosis of necrotising fasciitis and rapid antibiotic treatment and surgery are critical in stopping this infection before it causes severe damage or death.
Causes
Group A streptococcus bacteria is one of the most common cause of necrotising fasciitis. Usually called strep A, this is the same bacteria that can cause strep throat and skin infections in people. (There are other types of necrotising fasciitis caused by different bacteria or fungi.)
Strep A are common bacteria found on the skin, including the skin near the anus, the genital tract, and the throat. They can enter the skin through cuts, lacerations, grazes, burns, insect bites, puncture wounds (including from needles and cannulas), and surgical wounds. Even minor wounds such as a prick from a rose thorn or a mosquito bite can allow Strep A through the skin. People can get necrotising fasciitis following blunt trauma that does not break the skin.
Not everyone is colonised by strep A all the time. It can come and go from skin contact with other people.
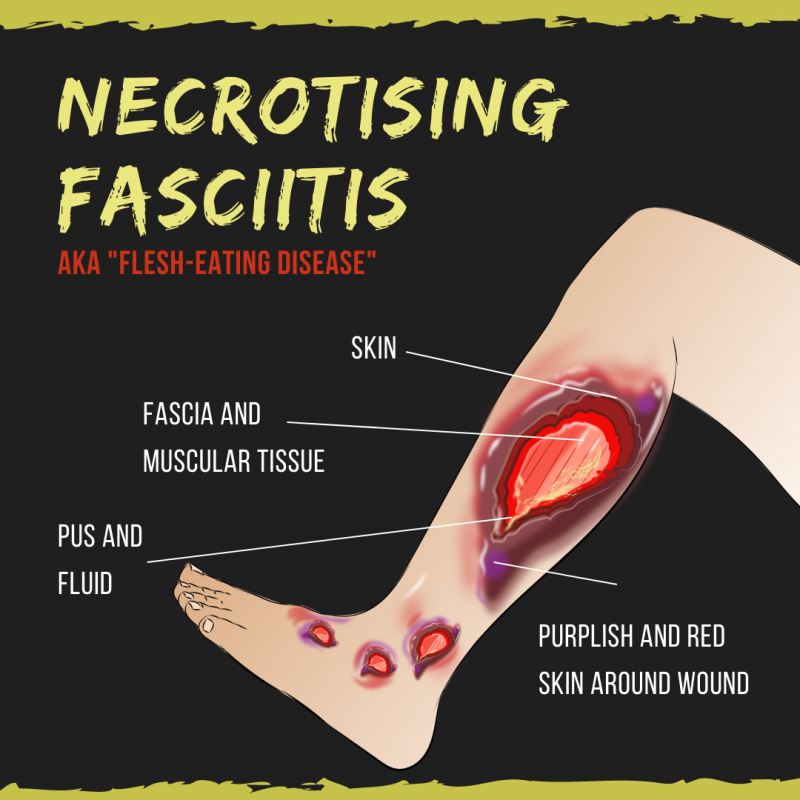
Symptoms
The most common site of infection is the lower leg. Necrotising fasciitis can affect upper limbs, perineum, buttocks, trunk, head, and neck.
Symptoms appear usually within 24 hours of a minor injury.
- A red, warm, or swollen area of skin that spreads quickly
- Severe pain, including pain beyond the area of the skin that is red, warm, or swollen
- There may be flu-like symptoms, such as nausea, fever, diarrhoea, dizziness and general malaise (feeling unwell).
Seek medical help as soon as possible if you have these symptoms after an injury or surgery.
Risk factors
Necrotising fasciitis is rare but certain factors may make people more prone to it:
- a weakened immune system
- diabetes
- kidney disease
- cancer
- skin lesions
- being elderly
- obesity
- chronic heart or lung disease
- steroid use
- alcoholism
- liver disease
- drug use
- it can be a rare complication of chickenpox in young children.
Diagnosis and treatment
Early diagnosis and treatment of necrotising fasciitis is key. It’s a very serious illness that requires hospital care, often in intensive care.
Doctors will examine your skin and perform tests. They may take a biopsy, or small sample, of the affected skin tissue. Blood tests are used to look for signs and types of infection, or muscle damage.
Doctors will try and identify which organism is causing the infection and treat it with high-dose intravenous (directly into a vein) antibiotics.
If the bacteria have killed too much tissue and reduced blood flow in the area, antibiotics may not be able to reach all the infected areas. Doctors will surgically remove the damaged infected tissue. Multiple surgeries are not unusual, and the patient may need blood transfusions. In some cases, amputations of one or more limbs may be necessary.
Vaccines
There are currently no vaccines to prevent strep A infections, including necrotising fasciitis.
Prevention
Good wound care is the best way to prevent bacterial skin infections, including necrotising fasciitis. You can look after most minor wounds yourself, keeping them clean and preventing infection.
You should see a doctor or nurse if:
- the wound is deep, including puncture wounds, or doesn’t stop bleeding when you apply pressure
- you can’t properly clean dirt and debris out of the cut
- the wound has dirt, a thorn, glass or other foreign body in it
- you have cut your hand from punching something
- the cut is over a joint
- the wound is more than a few millimetres deep and/or the sides of the cut don’t sit together well by themselves (a gaping wound). These may need closing with stitches, tissue glue or staples
- the wound is in or near your eye or is on your eyelid and is not shallow
- you notice changes around the wound, such as spreading redness, increasing pain, tenderness or swelling, or it starts oozing pus
- you develop a temperature
- the wound is from a bite, whether by an animal or human
- the wound is contaminated with soil or saliva, or happened in dirty water
- you have diabetes
- you’re not sure whether you’re up to date with your tetanus shots
- you have a wound that’s not healing or is very slow to heal.