
Did you know your heart is like a car engine?
My Amazing Body is a podcast where we explore interesting, unknown and misunderstood parts of your body with help from medical experts and stories from real Queenslanders.
This episode is all about the heart. Dr Greg Starmer, the Director of Cardiology at the Cairns Hospital explains what the heart is, what it does and why it’s so important. He also talks about problems that can occur with your heart and the best way to keep it healthy. Amanda, a Queensland woman, talks about what it’s like to live with a pacemaker.
Meet our guests

Episode materials
Audio is great, but some things are best seen as well as heard, or might tempt you to do further reading. These materials provide more information about topics we touch on in the show.
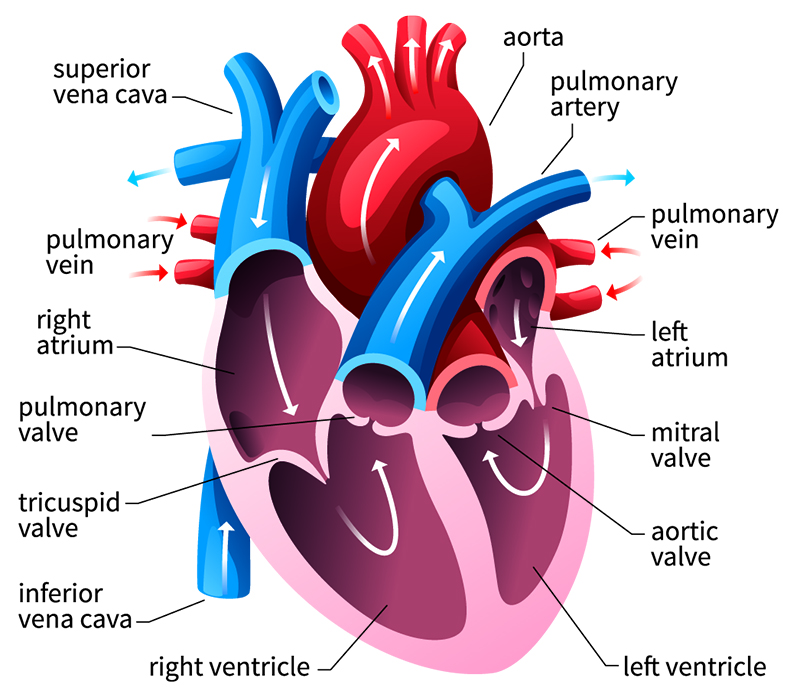
The heart
Heart disease and keeping your heart healthy
In this episode, Dr Starmer talks about how to keep your heart healthy. You can find more tips for heart health at the links below.
Health Direct: 5 ways to reduce your risk of heart disease
Heart and cardiovascular conditions
Queensland Government: Heart health
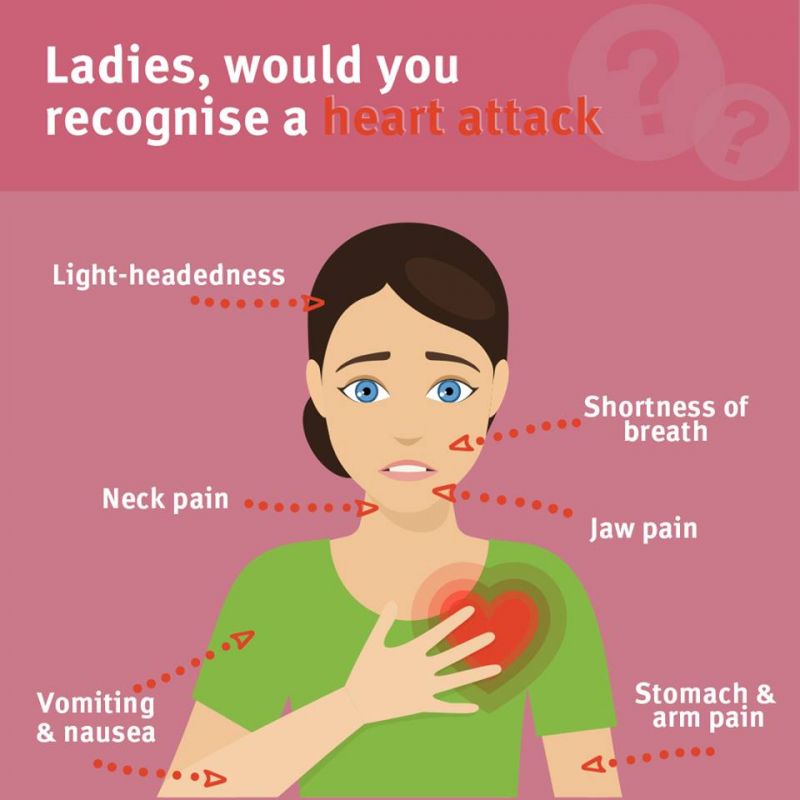
Signs of a heart attack can differ in men and women
Chest pain is thought to be the most common symptom for a heart attack – and it is common in men. However, only about half of all women who have a heart attack actually report having chest pain.

The arteries and veins
For more information on arteries and veins listen to episode 12 from season one of My Amazing Body
Episode transcript
Dr Starmer: The heart I think is... It's a fascinating organ for several reasons. I think we place a lot of importance on the heart as we should because you only have one and it's got a very important job to do. And perhaps I'm oversimplifying but it's a relatively straightforward organ with a straightforward function,
Host: That's the Director of Cardiology at the Cairns Hospital, Dr. Greg Starmer. He is talking about your one and only heart. Arguably, the most important organ in the body.
Welcome to this episode of My Amazing Body, a podcast where we explore interesting, unknown and misunderstood parts of your body. Today, we're learning all about your heart.
What exactly is the heart? What does it do and how does it work? Dr Starmer says that the heart is like the engine of a car. And you’re the car.
Dr Starmer: The heart is essentially the engine of the body so it is a muscle much like your legs or biceps and it is responsible for pumping essentially blood and nutrients around to your lungs to get oxygen. And then to all other parts of your body, the cells, to provide that nutrient, and energy and oxygen, so that it can be utilized. So, effectively it's like the car engine. It distributes what is required from one area to another.
The heart has four chambers. There is two powerful pumping chambers at the bottom of the heart and the one on that right side, that one's responsible for getting the blood up to the lungs where it receives its oxygen. And the bottom chamber on the left is a very powerful chamber. That's the one that we all really care about and that sends blood around the entire body, up to the head first.
It's responsible for feeding itself, so it sends blood down little arteries to itself first to ensure that it has its own nutrient supply. And then all the way down to your kidneys, liver, muscles, all the way to your toes and back again. There are two chambers at the top of the heart that sit above those two powerful pumping chambers. So, one on the right and one and the left, and they're effectively reservoirs. They contribute a little bit of kick, we call it the atrial kick because they're called atria. But they effectively receive the blood on the right side from the rest of the body. And on the left side from the lungs before it falls down into those powerful pumping chambers at the bottom.
Host: If you place your hand on your chest, you'll be able to feel your heart beating. It's busy pumping the blood around your body. But, how and why does it beat and what is your pulse?
Dr Starmer: It beats because it's got an electrical system. So, much like the wiring in your house, the heart has a generator and that sends electrical signals down to a relay station, which is situated pretty much right in the middle of the heart. And then, via really three huge electrical cables, two to the left and one to the right, down to those pumping chambers at the bottom of the heart. And as I said, it actually still needs its own energy and oxygen supply to make it work and work efficiently and as soon as the blood exits the heart, the heart, reasonably so, is relatively selfish and the first thing it feeds is itself. So, blood then falls down little fuel lines, I guess, called the coronary arteries, which feed the heart with the nutrients and energy it needs to do its job.
The pulse rate is effectively your heartbeat. So, your heart beats and then as it squeezes, that sends this blood rush like a tidal wave, it's like a tsunami-like tidal wave down throughout your body and we feel that as a pulsation. So, at your wrist, sometimes in your temples, you feel that as a pulsating. So that's when your heart is squeezing, that's when it's beating. It's sending this pressure wave of blood throughout all of the vessels in your body. And in between, you get a little lull in that and that's why you have a gap because the heart's filling, it's not squeezing.
Host: Your heart is about the size of your fist and while most of us think it sits on the left side of your chest, Dr Starmer explains, that’s not entirely correct.
Dr Starmer: A lot of people think the heart is kind of on the left side and it sort of angles that way. But really it's directly behind the breastbone. So we're built fairly well and the reason that we're built the way that we're built is to protect the heart and the great vessels that enter and exit the heart. So, it's predominately behind the breastbone with a little sort of angulation over towards the left side. It usually is about the size of your fist I guess, perhaps a little bigger and that's in an adult of course. But that can vary depending on the size of the person, whether they are an athlete... So some athletes will have slightly larger chambers and muscular walls.
Host: The heart is very well studied, and we know a lot about how it works. Dr Starmer says its solutions to heart problems or conditions that we are still learning about. You may have heard of some, a heart attack, heart failure, angina, or even a hole in the heart.
Dr Starmer: There's a multitude of things that can affect the heart but fortunately, particularly in this part of the world in Australia, we're very lucky. It's been very heavily researched, and we've got a lot of treatment options available.
Host: Did you know that babies are almost always born with a hole in your heart? Problems arise when the hole doesn't close up after birth and sometimes an operation is needed to close it.
Dr Starmer: A hole in the heart is something that you're almost always is what you're born with. In fact, before we're born and when our heart is being built and when the rest of us is being built, there is one key difference between that part of the human and the post- birth I guess baby and that is the lungs. And before we're born, we're not taking any breaths and therefore there needs to be a way to get blood from the right side of the heart, once it's been used if you like, over to the left side of the heart and to recirculate through the areas that is required.
Now, normally that would go via the lungs but before we're born, we're not breathing. So, there is typically a connection across there and that usually closes up in the first three days of your life. So, you take a breath, and then all of a sudden there's this big pressure shift and that hole in the heart will close. Sometimes though, and in fact, in that particular type of situation, up to one in four people may actually have a little residual opening there. There are some other situations as well where some of the connecting wall between those two chambers just doesn't quite form completely. So, there can be little gaps and little holes and if they're very small, there generally is no problem at all.
Host: One of the most common conditions of the heart in adults is coronary artery disease. Dr Starmer explains that it is all about cholesterol and plaque build-up in your arteries.
Dr Starmer: So, this a disease that affects the little fuel lines that supply the heart with blood and nutrients and this is the most common cause of death in the western world. So, it's a very, very common problem, and trying to fix these fuel lines, trying to remedy the situation has become one of the most common procedures that occurs in the medical world. So, this really all stems back to plaque or atherosclerosis and cholesterol. And it's this cholesterol build up within these little fuel lines, these little rivers of blood to the heart that cause so much trouble. And once certain things occur, whether it's smoking, diabetes, high blood pressure, diet and exercise, or poor diet and exercise, and even genetics plays a significant role and that can lead to a build up of cholesterol plaque in the arteries. And what you generally encounter at that point is an imbalance between supply and demand.
The heart is as I said, it's a muscle and it needs its energy, it needs blood. And the harder you make it work, for example, by running or cycling or swimming, whatever you want to do, the more it will demand. The more energy, the more fuel you need to feed it. And if there is a fixed obstruction, so if the pipe has a narrowing in it, then it won't be able to receive the energy that it needs and that will cause certain areas of it to be starved and that can lead to angina, what we commonly know as angina, which is a tightening of the chest.
Host: It's a misconception that women don't suffer heart attacks. Dr Starmer says, they do and it's about knowing the symptoms which can be different in males and females.
Dr Starmer: The heart attack is a problem with those little coronary arteries, the fuel lines to your heart. So they run over the surface of your heart and when they get blocked, they cause heart attacks and that can be a big problem. That can lead to areas of the heart that don't work very well and if you have enough of those areas of the heart that don't work very well, then that can lead to heart failure.
The presenting symptoms do seem to be different. So, males are more likely to present with the usual sort of triad of central chest discomfort, very heavy in the chest, sweating sometimes, and breathlessness. Maybe tightness up into the jaw radiating down the left arm, things like that are very, very classical symptoms and they tend to be very common in a male presenting with a heart attack.
Females on the other hand do have a much higher rate. So, they do still present in a similar fashion a lot of the time. However, they have a much higher rate of presenting with what we call atypical symptoms. So, that is more commonly with breathlessness rather the tightness. It may be just a sort of feeling of general unwellness even. There may be dizziness, light-headedness, or even a feeling of nausea.
Host: We spoke with Amanda, a Queenslander who presented to the Prince Charles Hospital emergency department with signs of a heart attack.
Amanda: I had shortness of breath, chest pains that led down my left arm and stiffness in my neck. When I presented to the hospital, they did a test and ruled out that it was a heart attack, that my heart was doing some really weird things.
Host: After a week in hospital and many tests the doctors discovered it was the electrics of her heart that weren't communicating properly. Dr Starmer says that this condition is more common as you age.
Dr Starmer: The heart has an electrical system and you can imagine if you had the same wiring in your house for many years, for 80 plus years, and sometimes when you switch the light on or you turn the switch on, the light wouldn't come on. And it's very similar. So, the longer you live, the more chances you will have to disrupt the electrical system in your heart. And that's where we start to think about things like pacemakers to effectively sort of replace the wiring in your heart with the wires that we have at our disposal at the moment.
Host: But for Amanda, who was only 41 at the time, it was thought to be something she was born with that, unfortunately had gone undiagnosed.
Amanda: they think that I was probably born with this, I guess, deficiency in my heart and just gone undetected all my life. They thought that as a child, my shortness of breath was asthma, so I had for a long time being diagnosed with asthma, using puffers. And it wasn't until five years ago, when I presented at the hospital with chest pains that they realized it was actually something to do with my heart and not asthma at all.
Host: Once discovering it was the electrics of her heart the doctor decided that a pacemaker was needed to fix the communication between the bottom and top part of her heart.
Amanda: I didn't realize that my shortness of breath that I've had all my life was actually the symptoms of electrics of my heart not working properly. So, I didn't get to go home after I presented to Prince Charles Hospital, so I spent the week in hospital and towards the end of the week. Well, it was a quick surgery and basically it is where they insert the pacemaker just underneath the muscles of the left-hand side of your chest, and they insert the wiring through and connect it through to your heart.
Host: Amanda says after the surgery it felt great to take a deep breath and that most of the recovery was done at home.
Amanda: I remember waking up after surgery and recovery and my husband said, "How you feeling?" And I'm like, "I didn't know it felt like this to have a good, deep breath in." I didn't realize because I'd lived with it all my life.
I was a little bit sore with my arm, I had two weeks off of work after that, couldn't really lift anything above my sort of shoulder height for the first two weeks and obviously just light duties when I was picking up things. So, sort of, I guess the best way to describe it was it felt like you'd torn a muscle because obviously they had to cut through muscle to put the pacemaker in, so it was just a recovery period time. But then once that was in, it was all good and it felt good to actually take a deep breath in and know what that breath should feel like.
Host: For Amanda the greatest lifestyle change post surgery was having to give up contact sport.
Amanda: You try and carry on with life as normal. For me, the only major change was is that I couldn't play any more contact sport, so I was quite into my netball and I had to give that away because you can't risk being hit in the chest. So, that was probably the biggest restriction that I had. But otherwise, most of your daily exercise, like if you went for a walk or anything like that is all normal.
Host: About a year ago Amanda started to feel unwell again, only this time it seemed like she might have been suffering from Ross River Fever.
Amanda: When I didn't recover properly after that, my bloods showed that I had Ross River fever but when I went for bloods a second time when I wasn't getting any better, they discovered that it wasn't Ross River fever and they had detected in my bloods that I had an auto immune disease but they couldn't figure out what it was.
I had many, many months, nearly a year of feeling unwell, swelling in my arms, in my face, shortness of breath, just genuinely feeling unwell before I ended up back at Prince Charles Hospital in March this year presenting with all that swelling, stiffness in my neck, just generally not feeling well. When they sent me for a CT scan, they found quite a few blood clots. And because of the placement of those blood clots, I then had to fall under not just a cardiologist but a neurologist and a vascular doctor as well. So, I was quite unwell and spent, I think, all up about four weeks in hospital before I was allowed to go home. And in that time, I had to be put on quite a lot of medication to thin my blood and dissolve some of those clots. And then obviously, COVID hit, so my assigned surgery was cancelled, which was to take the pacemaker out because all of those symptoms that I was feeling, even though it went undetected, was my body rejecting the pacemaker.
Host: Normally, if your body is going to reject the pacemaker it would be in the first 12-18 months. It's uncommon for your body to reject a pacemaker five years down the track.
Amanda: But what they think is that whatever I contracted at Easter last year was a virus, and then my body didn't really recover from that and that's how they think that some of these clots started for me. And I guess had I been sent back to my cardiologist in the earlier stages, I may not have needed the surgery that I had this year, it possibly could have been fixed with some medication and monitoring. But unfortunately, because my doctors and specialists were looking for an auto immune disease, I didn't get sent back to my cardiologist.
Host: This time Amanda needed to have two surgeries, one to remove the old pacemaker and one to put the new one in place.
Amanda: I had to undertake two surgeries, pretty scary because it was in the time of COVID. So when they allocated my first surgery, COVID was very at its peak and my surgery got cancelled, but then we got notification saying that category one surgeries would still go ahead and I was classified as category one, so I got a phone call four days later to say that my surgery would be going ahead. And that surgery was to remove the pacemaker that was already in, which is a very risky operation to do because having the pacemaker in for the five years, those pacemaker leads, your body normally starts accepting them like a normal vein and so your normal body parts start to attach themselves and grow over those wires. So, it's a very risky operation to take out a pacemaker that's already in.
Host: Before they could change the pacemaker doctors needed to make sure Amanda's heart could handle the new technology.
Amanda: It's a different pacemaker that I have this time. So, before they took the pacemaker out that I had five years ago, they sent the pacemaker clinic up to me in hospital and they readjusted the settings of my existing pacemaker to see whether I could cope with it pacing at this new style of pacemaker. The new style of pacemaker that I have is leadless, which means that it only paces the bottom part of my heart. I had enough because obviously the old pacemaker paced the top and the bottom chamber and this new one only does my bottom chamber.
But it's a very different surgery for the second one, the new one is very tiny. And because it's wireless, it's actually not inserted in the top of your chest, it's actually done via a vein in your groin, so very similar to an angiogram.
Host: After the surgery Amanda was able to go home the very next day. She, and her doctors, are hopeful that the new technology will reduce the chances of her heart rejecting this updated pacemaker.
Amanda: Yeah. And so therefore my recovery for that one was a lot quicker because they're not going through muscle or anything like that. I actually felt quite good after that operation and I was keen to go home. I went into surgery late in the afternoon and I was home the next morning.
The pacemaker, the new one, sort of has a battery life between eight and 10 years, so I guess it just depends on how often that kicks in as to what your battery life is like. So, you go for six monthly checks at the start and then the pacemaker clinic, if they're happy with it, will decide whether they want to change you to 12 monthly checks, or you're referred back to your cardiologist. Yeah. But as far as anything else, it's all pretty good and try and get back to normal life.
Host: Are you enjoying this season of My Amazing Body? If you like it, why not tell others, by leaving a rating or review in your podcast app, or sharing that you're listening on socials.
Are you ready for this episode's mystery body part? See if you can guess the body part from the clues given. We'll reveal the answer at the end of the episode.
I have a lot of hair follicles.
I am among the warmest areas of the body.
Blood and lymph vessels travel through me.
I'm also known as the axilla.
Do you know what I am?
Adrenaline or stress can be crucial in activating your fight or flight response, but a lot of stress isn't great for your heart.
Dr Starmer: Stress is certainly something that can cause problems. There is a lot of research into this area as well. Stress causes different types of problems with your heart is probably the best way to put it. So, in terms of heart attacks, stress can induce a particular type of syndrome if it's a sudden stressful event and we call that takotsubo, which means octopus pipe in Japanese, which is what the heart looks like when you have one of these hugely stressful events and the heart deforms and changes shape. And in many ways mimics a very large heart attack. Now, fortunately, in those types of people, if you can get through those initial stages which most people do with modern therapy, it all completely recovers.
Stress can... Also, makes your blood pressure so it causes little neurochemicals, things like adrenaline in your body to go up and that is effectively a whip for your heart. So that makes your heart work harder, it squeezes down on the blood pressure... On the blood vessels in your body, which is what we need sometimes when we're frightened, and we need to get away from something dangerous. But you don't want to have that all that time because that can lead to higher blood pressure and that puts your heart under increased load as well.
Host: Have you ever wondered why your heart rate goes up when you exercise? Dr Starmer explains that it's similar to putting your foot on the accelerator when you are driving up a hill.
Dr Starmer: When it comes to getting the heart rate building up, it is again... I always, I know I keep coming back to it, but it's very similar to the engine analogy. So, if you need to get that car up a hill or if you want to overtake someone, then you really need to put your foot on the accelerator and you're making the engine work harder and therefore you see that little needle going on the RPM, the revolutions per minute, it might go from 2,000 to 3,000, 4,000, whatever's required to get you to do what you need to do to get past that car, over that car or whatever's required. And it's very similar with the human heart.
So, if you need to do something, if you need to exert yourself more if you need to get up a hill or you're pushing yourself to complete a race, then your body will need and demand more, it will need more. And once your heart has hit its sort of maximum output then the only way that you can get more is by increasing your heart rate. So, we talk about the output of the heart, that's the most important thing and that is depending a little on what we call the stroke volume, which is the amount of blood that it can squeeze out. But once that hits its limit, it really is completely dependent on the heart rate to increase what it needs to get around, to get that energy to where it's needed. So, that's generally why we see our heart rate pick up when we need to exert ourselves, just to supply the body with what it needs.
Host: We only have one heart, so it's important we known how to look after it. And it's actually very simple.
Dr Starmer: It's not particularly complicated, it really boils down to healthy living. So, smoking is absolutely a disastrous thing you can do for your heart and your body in general and that... And all forms of illicit drugs have detrimental effects on your heart. So, no matter your beliefs on the other things, they absolutely have serious untoward effects on your heart. But then it really does come down to simple things like diet and exercise. Exercise is crucial and it can be... Really what I say is it's whatever you can do and sustain and then generally, people will build from there.
Diet is also crucially important. I guess the problem with diet these days is there's so many different types of diet. But what it comes down to is maintaining a healthy body weight and making sure that you avoid the things that we know are bad for your heart. So, refined sugar, so there is no reason for soft drinks and I mean I don't mind the odd chocolate cake at a birthday but you really have to burn that off and earn it if you're going to indulge every so often. And these should be sort of very, very occasional treats and they have to be coupled with exercise to get rid of that refined sugar otherwise it will be just stored as fat and that fat will end up in the arteries of your heart, unfortunately, and that brings me to saturated fats as well.
Everything that we put into our bodies is a potential, or most things we put into our bodies is a potential energy source and that's what eating is. It's about providing energy and if we don't use that energy then that will be stored somewhere, we don't want it to be stored. So, the best thing you can do is have a healthy diet very low in fat and particularly low in refined sugar and then ensure that you spend that energy. So, whatever you are doing, you exercise to use that as a counterbalance. And if you find that... I always say if your weight is going up then it's supply and demand so one of those things will have to change.
Host: Dr Starmer says he feels very fortunate to be able to build strong doctor-patient relationships in his job.
Dr Starmer: We have a very large population of First Nations, Aboriginal, and Torres Strait Islander people and I think establishing a relationship is important. And I genuinely love that element of my job. I love talking to people, hearing their story, hearing where they're from, and then doing what I can to make their life even just a little bit better. So, if I can achieve that, then I'm happy.
Host: Thanks for listening to this episode of My Amazing Body. Before we go, did you guess the mystery body part? The axilla is your arm pit. Congratulations if you figured it out.
Thank you to Dr Greg Starmer and the team at Cairns Hospital and Health Service for telling us all about the heart, and thanks to Amanda, for sharing what it's like to live with a pacemaker.
My Amazing Body is brought to you by Queensland Health. Many thanks to my colleagues: Lauren and Jess our producers, Carol our sound technician and Helen on music and sound effects.
