Syphilis outbreak in Queensland
On this page:
- Syphilis in Queensland
- Queensland Infectious syphilis outbreak
- Clinical management
- Queensland Syphilis Surveillance Service
- Syphilis surveillance and reporting
- Information, guidelines and resources
- Syphilis campaigns
- Training
Syphilis is a curable multistage disease caused by bacteria of the species Treponema pallidum, subspecies pallidum, that can cause serious health problems if left untreated. Syphilis is usually transmitted during anal, oral or vaginal sex through skin-to-skin contact with an infected area or through vertical transmission from mother to child. There are 4 stages of syphilis infection: primary, secondary, latent and tertiary. Each of these stages presents with different signs and symptoms.
Infectious syphilis is a significant public health concern, particularly due to the risk of congenital syphilis. The risk of vertical transmission from mother to child is high for untreated infections, with the risk diminishing over the years but never disappearing. Syphilis can also increase the risk of HIV infection, as syphilitic genital ulcers provide a portal of entry for HIV acquisition and a focus for HIV transmission.
Syphilis in Queensland
Between 2001 and 2023, the rate of infectious syphilis notifications in Queensland increased nine-fold from 3.1 to 26.4 cases per 100,000 people per year (see Figure 1).
First Nations populations and gay, bisexual and other men who have sex with men (GBMSM) continue to be disproportionally affected. Since 2016, notifications have substantially increased among both First Nations and non-First Nations heterosexual males and heterosexual females of reproductive age with a subsequent increase in congenital syphilis and adverse pregnancy outcomes.
Between 2001 and 2023, 50 cases of congenital syphilis were reported in Queensland, 35 of which were in First Nations infants. Of these, 17 were associated with intrauterine foetal death/stillbirth or the babies died after birth (16 First Nations and 1 unknown First Nations status).
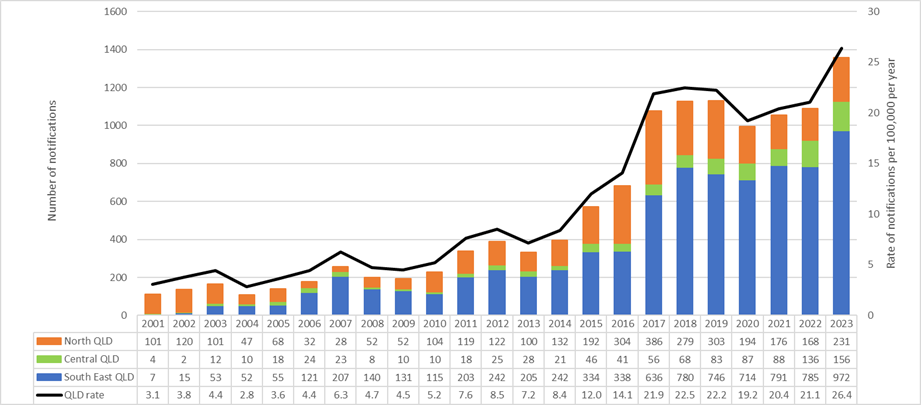
Figure 1: Number and rate of infectious syphilis cases in Queensland*, 2001-2023, by region.
*North QLD: Torres and Cape, North West, Cairns and Hinterland, Townsville, Mackay. Central QLD: Central West, Central Queensland, Wide Bay, South West, Darling Downs. South East QLD: Sunshine Coast, Metro North, Metro South, West Moreton, Gold Coast.
Queensland infectious syphilis outbreak
There is an ongoing infectious syphilis outbreak affecting young First Nations people living in Queensland, the Northern Territory, South Australia, and Western Australia, particularly in rural and remote areas.
Increased syphilis numbers were first observed in Queensland’s North-West Hospital and Health Service (HHS) in January 2011. An outbreak was declared in the area in September 2011 and subsequent outbreaks soon declared across four of the five North Queensland HHSs.
In recent years syphilis notifications have substantially increased across Queensland’s South-East corner and major cities coinciding with the increase in heterosexual transmission among First Nations and non-First Nations populations of reproductive age. In 2021, the Chief Medical Officer issued a communique to health professionals advising of this expansion of at-risk groups.
The syphilis outbreak has continued to spread to other states and territories with the entire northern and some parts of southern Australia now affected.
Clinical management
Timely and adequate testing and treatment for syphilis (including during pregnancy) and contact tracing of sexual partners are paramount for reducing notifications, risk of infection and burden of disease.
For all pregnancies, it is recommended to get tested for syphilis during routine antenatal screening; at the first antenatal visit, at 26–28 weeks, and again at 36 weeks gestation, per the Queensland Syphilis in Pregnancy Guideline. Patients at risk of inadequate antenatal care are to be screened opportunistically and additional testing, including at birth, should be considered based on clinical indication.
Clinicians are also encouraged to take a sexual history, discuss prevention and initiate STI testing for all sexually active patients, including syphilis serology, particularly if any ulcers around the mouth, anus or vagina or rashes are present. Symptoms, if present, will vary across the stages of syphilis infection. More information on testing, symptomology and treatment can be found in the Australian STI Management Guidelines.
Infectious syphilis treatment alert
It is crucial to note that the correct first line treatment of infectious syphilis is Benzathine benzylpenicillin (trade name Bicillin L-A). Aqueous benzylpenicillin (trade name BenPen) is not a suitable treatment. For more information about the important differences, please see factsheet: Benzathine benzylpenicillin is not ‘BenPen’ (PDF 231 kB).
Australia is currently experiencing a shortage in the availability of prefilled Bicillin L-A syringes. More information on alternative treatment whilst conserving Bicillin (or when Bicillin is unavailable) can be found in this clinical care alert.
Queensland Syphilis Surveillance Service
The Queensland Syphilis Surveillance Service (QSSS) (North and South Queensland teams) reviews all notified syphilis cases. They provide the treating clinician with information about a patient’s history of syphilis testing and treatment to support the accurate staging of infection and clinical management. The service also plays a key role in enhanced surveillance data collection, and education on syphilis, and may assist with contact tracing.
Phone: 1800 032 238
Email:
- South Queensland Qld-syphilis-surveillance-service@health.qld.gov.au
- North Queensland North-qld-syphilis-surveillance-centre@health.qld.gov.au
Syphilis surveillance and reporting
Syphilis is a notifiable sexually transmissible infection (STI) in Queensland under the Public Health Act 2005 and Public Health Regulation 2018 with all laboratory-diagnosed positive syphilis test results being notified to the Notifiable Conditions System. Publicly available communicable diseases data is reported weekly at different levels across Queensland and is used to investigate local notification totals and trends.
Queensland Health produces reports describing notifications of syphilis in Queensland, focusing particularly on the demographic distribution and risk factors among infectious syphilis and congenital syphilis cases.
- Syphilis in Queensland 2022 report (PDF 2756 kB)
- Syphilis in Queensland 2021 report (PDF 9225 kB)
- Syphilis in Queensland 2019 report (PDF 639 kB)
- Syphilis in Queensland 2010–2015 (PDF 838 kB)
The Multijurisdictional Syphilis Outbreak Working Group (no longer active), formed by the Communicable Diseases Network of Australia in April 2015, also produced regular surveillance reports summarising national epidemiological data from the outbreak for the period 2016–2020.
Information, guidelines and resources
- Syphilis fact sheet
- Sexual health conversation starter sheet for GPs
Case report forms:
- North Queensland Syphilis Case Report Form (PDF 249 kB)
- South Queensland Syphilis Case Report Form (PDF 224 kB)
Testing and management tools and guidelines:
- STI/BBV Testing Tool for Asymptomatic People (PDF 639 kB)
- Queensland Clinical Guideline – Syphilis in Pregnancy (PDF 558 kB)
- ASHM syphilis decision-making tool
- Australian STI Management Guidelines
- National case definitions for infectious syphilis, syphilis unspecified and congenital syphilis
- Series of National Guidelines (SoNGs) - Syphilis
Syphilis campaigns
- Lady Peeps raises awareness among women about syphilis, particularly during pregnancy. The campaign encourages all women who are sexually active to take control of their sexual health and seek regular STI tests that include syphilis.
- Young, Deadly, Syphilis Free campaign is a multi-strategy STI awareness-raising campaign developed in response to the ongoing syphilis outbreak affecting Aboriginal and Torres Strait Islander communities, with a central focus on encouraging young people aged 15 to 34 to get tested and treated.
- Let’s treat syphilis is a campaign developed by Queensland Positive People and Queensland Council for LGBTI Health aimed at increasing awareness about the rapidly rising rates of syphilis in Queensland among GBMSM.
- Don’t fool around with syphilis is a national campaign launched to raise awareness of syphilis and the current multijurisdictional outbreak.
- WA syphilis outbreak awareness campaign was developed in response to the outbreak of syphilis in the Perth metropolitan area and aims to raise awareness of syphilis in women and encourage STI testing of females aged 16–40 years.
- Respect Me + You, Is Your Syphilis Check Up Due is a collaboration between the Aboriginal Health Council of South Australia and SHINE SA that promotes the message of staying connected and getting tested for syphilis.
Training
- Antenatal Sexual Health Kit (ASK) training for antenatal clinicians—understanding syphilis and congenital syphilis risk, undertaking sexual health assessments and initiating contact tracing in a maternity context.
- Syphilis Outbreak Training—this syphilis training website provides integral professional development for any health practitioners working in areas affected by the syphilis outbreak including doctors, nurses, midwives, and Aboriginal and Torres Strait Islander Health Workers.
- Introduction to Syphilis Nursing—this online learning module is designed to provide nurses with knowledge of priority populations for screening and testing, appropriate testing, interpretation of serology and contact tracing to reduce syphlis infections in Australia